Sources
There’s pork insulin which is almost nonexistent at this point. Pork insulin differs from human insulin by only two amino acids.
Most of the insulin is now bio-genetic insulin (“human insulin”) which comes from E. coli bacteria. Human insulin is now cheap enough to drive pork insulin out of the market although it’s still available.
Reactions: Lipodystrophy can develop, which is a fat bump under the skin that occurs from constantly injecting from the same place. To prevent this you must rotate the injection sites.
Varieties
U-100: When we administer insulin, we administer it in units. Insulins can come in a variety of unit concentrations but most of them are U-100 insulin. That means 100 units per milliliter. If you look at an insulin syringe, it has number markings on it. Those numbers indicate the units. 1 unit is a tenth of a cc. (1 unit = 0.01cc)
U-500: There’s another type of insulin you may see a couple times a year in your patients which is a U-500 insulin. That’s 500 units per ml. These patients have a severe form of diabetes that requires more than 100 units of injection. If the patient needs 150 units of insulin, you don’t want to use two injections, so you would use U-500 insulin, which is five times more concentrated and can fit into one syringe.
When a pharmacy sends a U500 vial to the nursing floor and it goes in the refrigerator, they put fluorescent stickers all over this vial to warn you that this is U500 insulin. If you draw up 30 units for a patient and it’s accidentally U500 instead of U100, that’s 150 units of insulin and they can become hypoglycemic and die.
Ultra-short acting insulin: Lispro (Humalog) works in a matter of minutes and just for an hour or two.
Rapid/Short acting insulin: Regular insulin works in a matter of 30+ minutes.
Intermediate acting insulin: NPH works for about 12 hours, so they’d need an injection twice a day. (Lente doesn’t exist anymore)
Long acting insulin: Works for 30 hours and some examples are Ultra-lente and Glargine (Lantus)
Recap
- Sources
- Pork, Bio-genetic (Human)
- Reactions: Lipodystrophy
- Varieties
- U-100 versus U-500
- Ultra-Short Acting: Lispro (Humalog®)
- Short Acting: Regular
- Intermediate: NPH
- Long Acting: Ultra-Lente, Glargine (Lantus®)
Regular Insulin
- The onset is less than 1 hour and it works for a few hours.
- We use regular insulin adjunct with longer acting insulin.
In the hospital you’d typically see NPH and Regular insulin being utilized together. The NPH will work for 12 hours and the Regular will work for a couple hours. The NPH won’t kick in right away, so in the morning when you give an injection before morning, you give them the regular insulin as well as the NPH. The regular insulin is clear. The NPH insulin is cloudy because it’s regular insulin bound up with a protein. When you inject it, our bodies immune system will break down this protein and we will eventually have the insulin. We always draw up the regular insulin first and then the NPH. If you draw up the cloudy NPH solution first, and then the clear solution, you may be pushing in some protein into the regular insulin vial and eventually the regular insulin becomes longer acting NPH insulin.
Intravenous: Regular insulin is the only insulin you could give intravenously. All the rest are subcutaneous. You could use this to treat ketoacidosis with an insulin drip. This is also useful during parenteral nutrition where they get their calories (protein, fat, electrolytes, trace elements) through a central line. Many patients can’t handle 35% dextrose and their blood sugar gets too high so they will also have insulin in this bag.
Sliding Scale
You’ll find orders written in a hospital setting that say:
Finger Stick Blood Glucose Test QID a.c. & hs (finger stick 4x a day, before meals and at bed time)
If blood sugar is 150-200 give 2 units Regular insulin.
If 201-250 give 4 units reg insulin.
If 251-300 give 6 units reg insulin.
If 301-350 give 8 inits reg insulin.
If 351-400, give 10 units reg insulin.
If >401, call for help.
Caution for glucose meters: These are not as accurate as hospital laboratories. These don’t work as well when the blood sugar is VERY low or VERY high and you can’t trust the results.
Recap
- Onset: less than 1 hour
- Uses:
- Adjunct with longer acting-draw up in syringe first
- Sliding Scale
- Intravenous: Treat Ketoacidosis
- Intravenous: Parenteral Nutrition
- Only Regular insulin can be administered intravenously
Intermediate Insulin
Onset is 2 hours. It peaks around 12 hours in and duration is 24 hours long. So they get a shot every 12 hours.
Long Acting Insulin
Onset is 3 hours and duration is 30 hours.
We give this at night since it takes time to kick in so that it’s working when it’s breakfast time.
All these insulin’s look similar
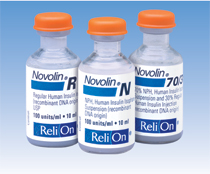 This is a huge problem. There’s two manufacturers of insulins: Elly Lilly and Novonortis. The Novolin R (Regular), Novolin N (NPH), and Novolin 70/30 all look similar so that is why we must be very careful and legally always needs two nurses to verify the medication.
This is a huge problem. There’s two manufacturers of insulins: Elly Lilly and Novonortis. The Novolin R (Regular), Novolin N (NPH), and Novolin 70/30 all look similar so that is why we must be very careful and legally always needs two nurses to verify the medication.
The 70/30 is very unique as it’s 70% NPH and 30% Regular. The manufacturer saturated the protein such that 70% is bound up but it cannot bind up the remaining 30%. For patients who can use this fixed ratio, the advantage is that they don’t have to draw up two vials of insulin.
Insulin Dose Variability
Every patient is different. When a patient gets into a hospital, that means they’re sick and there’s physical stress on their body which means there’s probably an excess release of corticosteroids, causing a high blood sugar level. The nurses deal with that either by a fixed number of units of insulin or a sliding scale.
If a patient has a severe infection, it takes about 3 days for their infection to go down. During this time the blood sugar level will be higher than normal and the insulin given must be varied to accommodate this. As the infection gets better, the stress goes down on their body. As the stress goes down, their insulin use must be decreased as well.






